ALCHEMY WITH THREE INGREDIENTS
With the LMO, there is a well-defined examination protocol to establish a precise diagnosis of the osteopathic lesions to be treated[1]. In short, treatment is derived from the osteopathic diagnosis which in turn is derived from the palpatory examination of the patient. Still’s formula, “find it, fix it and leave it alone”, implies at the onset: search! Before discussing an osteopathic method of diagnosis and treatment, it is therefore necessary to clearly define what we are searching for…
[1] But no protocol of treatment based on the patients’ complaint or medical label.
Somatic dysfunction or osteopathic lesion
The term somatic dysfunction officially replaced the term osteopathic lesion in 1968. To avoid any ambiguity in relation to an organic lesion in the conventional sense of the word, medical authorities at that time[1] abandoned the term osteopathic lesion for somatic dysfunction.
The diagnostic criteria of somatic dysfunction[2] thereby satisfied both Medical Doctors, advocates of official medicine, and Doctors in Osteopathy, proponents of functional medicine. In the wake of this seemingly trivial semantic concession, osteopathy became more interested in dysfunction itself rather than in the structural cause of the problem (the lesion).
To recapture the essence of osteopathic medicine with an aim to treat the structure in lesion to restore function (rather than the opposite), we must go back to the original and exact meaning of the term osteopathic lesion.
The osteopathic lesion (Latin : laesus, from laedere : injure), as was perfectly understood by the first osteopaths[3], is an injury that alters connective tissue. It evolves along the pathophysiological process of inflammation (acute phase) and fibrosis (chronic phase). It imprints in the structure a tissue scar that is palpable and therefore, manually diagnosable.
Any osteopathic lesion may of course generate a number of dysfunctions, both locally and at a distance, but we must not confuse dysfunction (the consequence) and lesion (the cause).
The term osteopathic lesion corresponds to objective tissue reality, and this is why we clearly prefer using this word (osteopathic lesion) rather than its substitute (somatic dysfunction).
[1] In particular the Hospital Assistance Committee of the Academy of Applied Osteopathy presided by Ira Rumney, DO. (Rumney I., 1969)
[2] Summarized in the acronym TART (Tissue texture change - Asymetry - Restriction of motion – Tenderness).
[3] A textbook of the Principles of Osteopathy, G. D. Hulett,, Journal printing company Kirksville MO, 1903
Characteristics of the osteopathic lesion
The two diagnostic criteria that allow to objectify an osteopathic lesion are:
- Loss of tissue elasticity with modification of suppleness of the point in lesion.
- Increased reactivity of the tissue with reflex response and, most commonly, increase mechanosensitivity of the point in lesion.
Tissue elasticity
Loss of connective tissue suppleness decreases the adaptation abilities of the body[1].
Any connective tissue of mesodermal origin may be involved: articular blockage, bony rigidity, ligamentous tension or distension, muscular contracture, visceral spasm, vascular or neural fixation, etc.
Take care not to confuse rigidity with density, as some do. Density is a physical characteristic specific to each structure. The increase of density in some parts of the body does not equate with an osteopathic lesion. Examples:
- we may find rigidity when applying a compression test to the neck of the femur (osteopathic lesion of an intraosseous line of force) in an osteoporotic elderly patient (decreased bony density),
- the osteopathic lesion of a soft tissue (organ, artery) may very well present more marked resistance to a tension test than a tissue of greater density does (bone, articulation),
- certain zones of the cranium are naturally more dense (lines of constraint) whereas others are less so. This in no way indicates the presence of osteopathic lesion.
Tissue reactivity
Any tissue injury affects[2] the nervous system and generates a motor, sensitive, sensory and/or autonomic neurological disruption. This neurological excitability brings about a defensive reflex of the tissue that is easily perceived by a trained hand through a tension test. Depending on the degree of “susceptibility of the tissue”, we may distinguish, through touch, two categories of osteopathic lesion.
- Active loss of elasticity, increased neurological vigilance with defensive reaction of the tissue: clear blockage, marked osteopathic lesion.
- Passive loss of elasticity, lesser neurological vigilance with slight defensive reaction of the tissue: sluggishness[3], osteopathic lesion of little significance.
We may compare osteopathic lesions to volcanoes; some are extinct (passive lesion) while others may possibly go into eruption (active lesion).
Active osteopathic lesions may only be found in the living[4].
[1] Possibly resulting in a disruption (either a restriction or an increase) of mobility of the affected structures.
[2] acute or chronic, in a silent way.
[3] Under his fingers, the practitioner feels a progressive resistance to the applied tension rather than a clear blockage. This type of fixation is most often adaptative.
[4] Cadaveric rigidity corresponds to a passive stiffening: there are no active lesions in a dead body.
Osteopathic diagnosis
The osteopathic diagnosis of the total lesion, of the dominant lesions and of the primary lesion[1] are derived from two original techniques: the tension test and the inhibitory balance test.
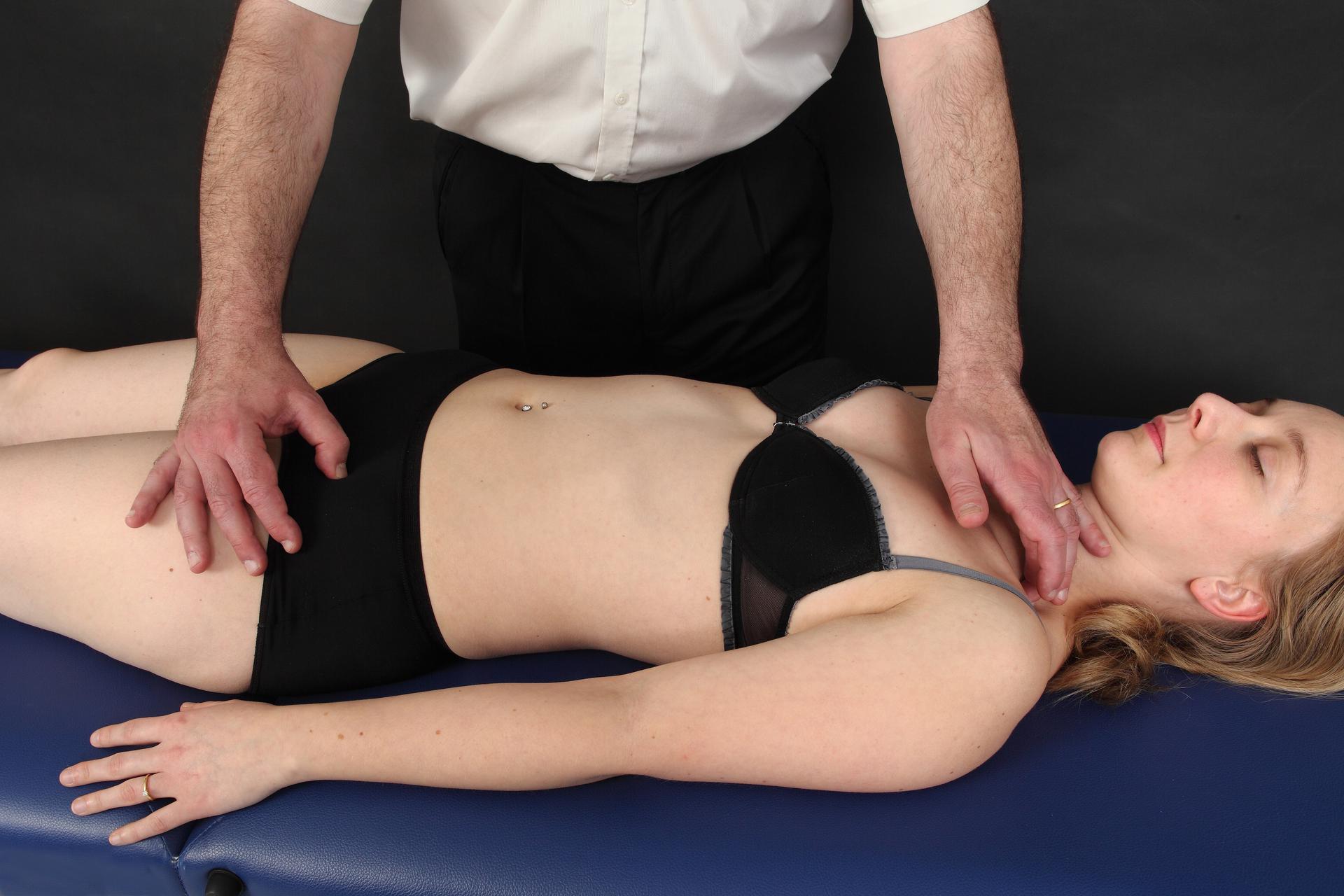
Tension test
The tension test consists of soliciting a given structure in a gentle and precise way to appreciate its elasticity. There is no mobilisation or “listening” to the structure but simply a direct evaluation of the suppleness of the tissue.
The tension test immediately yields three possible responses to the practitioner’s hand.
1) Tissue suppleness (normality)
2) Moderate resistance (passive lesion)
3) Clear and marked blockage which is the hallmark of a true osteopathic lesion (active lesion).
Thus, using the tension test, the operator perceives simultaneously a physical parameter (loss of elasticity of the tissue) and a reflex parameter (tissue reactivity).
The distinction between active and passive resistance results in a preselection of the lesions found so that only really significant blockages remain[2].
Depending on what is sought, there are several variations to tension tests: using pressure, traction, circumduction or compression.
The tension tests we propose have been found to be objective, reliable and reproducible[3]. This objectivity of the tension test gives credibility to the osteopathic diagnosis. Incidentally, the subject also feels perfectly well the different points of blockage that he exhibits when the practitioner applies his finger to them. The fact that the practitioner is able to find older and often forgotten lesions, without any interrogation and only as a result of his examination, never fails to amaze the patient[4].
Because they are quick[5], precise and comfortable, it is possible to apply a great number of LMO tension tests. For example, it is possible to perform a detailed evaluation of the entire spine and posterior thorax in only a few minutes and achieve a prioritized diagnosis of all the osteopathic lesions that are present[6].
[1] These terms are defined in the article: Mechanical Link: foundations.
[2] On average, a patient may present between 10 and 15 active lesions. If we were to add all the passive fixations, we would easily go over 50 lesions. The practical necessity of preselecting the lesions is therefore easily understood.
[3] Reliabilitätsstudie über die Befunderhebung der Wirbelsäule nach der Methode der Lien Mécanique
Ostéopathique, Claudia Hafen-Bardella, Ostéopathe M Sc DO. Burgdorf, November 2009.
[4] Also, it gives him confidence in the treatment he is about to receive.
[5] Comparatively to other processes of evaluation in osteopathy such as mobility tests or tissue listening tests which require more time in their execution.
[6] The complete examination of the patient requires approximately 500 basic tests (to which up to 200 optional tests may be added as required). A great number of tests are performed in a symmetrical and bilateral manner, which saves time. For a seasoned practitioner, the general examination takes 15 to 20 minutes and fits within normal consultation times (especially since the treatment as such will be very short).

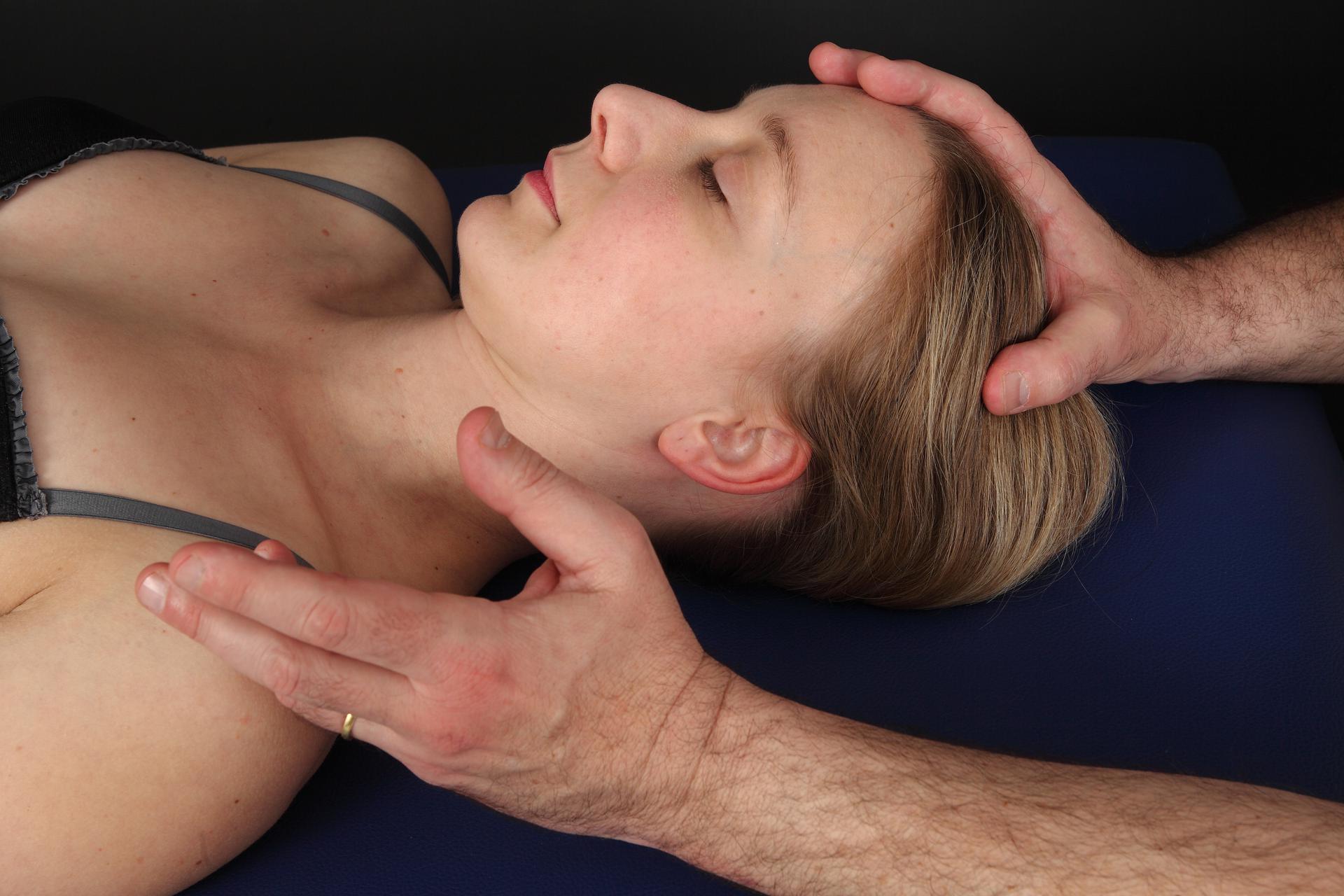
Inhibitory balance test
The inhibitory balance test, second step of our examination after the tension test, consists of comparing between the diagnosed osteopathic lesions to define which ones are worth treating.
To this end, the practitioner applies light and simultaneous tension to both fixations. A reflex then occurs immediately: one of the two lesions releases under the hand whereas, conversely, the other resists[1]. The inhibitory balance test requires a more subtle and lighter touch than the tension test[2].
This prioritization or hierarchy of lesions establishes a selection between the dominant lesions (most reactive) and the secondary lesions (less reactive). The lesion presenting the greatest degree of active resistance, in other words, the most “disruptive” of the lesion pattern, is considered as the primary lesion. It will of course be the first lesion to be treated[3].
In practice, there are two steps to the procedure of selecting the lesions.
- Prioritization of the different lesions within each functional unit (spine, periphery, viscera, cranium, etc.) to determine the most active: the dominant lesion of the functional unit in question[4].
- Prioritization among different dominant lesions of each functional unit (spine, periphery, visceral, cranium, etc) to determine the most active among them: the primary lesion (in other words, the dominant of the dominants).
[1] On the topic of hypotheses regarding the physiological mechanism explaining the inhibitory balance test, you may read: Inhibitory Tests as Assessment Tools for Somatic Dysfunctions; Mechanisms and Practical Applications, 2020 Bicalho et al. Cureus.
[2] The training of the hand can only be achieved through adequate learning. See the article entitled LMO Courses.
[3] The end of the diagnosis (the primary lesion) coincides with the beginning of the treatment (the first lesion to be corrected).
[4] It is possible to come across a functional unit presenting no lesion, or only one. In either case of course, no inhibitory balance test is needed.
Osteopathic treatment
On reconnait immédiatement un praticien du LMO parce qu’il utilise pour le traitement ostéopathique une technique de correction très particulière, étonnante, et qui parait un peu « magique » : le recoil ! Présentons ici cette technique mal connue et souvent mal comprise.
Le recoil
Le mot recoil vient de l’anglais recoil signifiant rebond, retrait rapide. L’origine du terme peut prêter à confusion car, comme nous allons l’expliquer, il ne s’agit pas de faire rebondir la structure !
Nous savons aujourd’hui qu’A.T. Still utilisait parfois une technique dont la description correspondrait au recoil, technique reprise occasionnellement par quelques successeurs (A. Becker, R. Miller) mais finalement tombée dans l’oubli[1].
Paul Chauffour a développé dans les années 1970 une technique originale qui consiste à induire une impulsion de très haute vélocité contre la résistance des tissus. Le recoil s’effectue d’une façon brève et très rapide mais, à la différence du toggle recoil ou du thrust, l’amplitude du geste est quasiment nulle[2].
On peut décrire le recoil en 3 temps:
1. Mise en tension avec recherche du point de résistance maximale.
2. Impulsion vive et directe contre la barrière tissulaire.
3. Retrait immédiat des mains pour laisser la vibration se propager.
Le recoil agit vraisemblablement au niveau des mécanorécepteurs dont les informations perturbées entretiennent la fixation des tissus, aussi bien localement qu’à distance (effet gâchette).
Le recoil combine avantageusement la correction structurelle (action mécanique) et la normalisation fonctionnelle (action neurologique) de la lésion ostéopathique. Notons que le concept actuel de biotenségrité justifie parfaitement tout l’intérêt du recoil dans une pratique ostéopathique moderne[3].
Le recoil permet d’ajuster sans restriction toutes les structures du corps humain : os et articulations, viscères, artères, nerfs, etc.
Le recoil convient à tous les cas, du nouveau-né à la personne âgée, du sujet en bonne santé au patient souffrant de pathologies lourdes.
Rappelons que le recoil n’opère pas de façon magique, ex opere operato, mais uniquement s’il est appliqué à bon escient, c’est-à-dire sur une lésion ostéopathique dont le diagnostic a été au préalable correctement posé. D’où la nécessité des tests de mise en tension tissulaire pour clairement identifier les fixations à traiter.
[1] Chauffour P., Prat E., Michaud J., Foreword to Mechanical Link arteries and autonomic nervous system by Steve Paulus, Sully 2009.
[2] On peut comparer le recoil à une frappe de karaté qui s’arrêterait juste au contact de la peau. Il y a bien un léger impact mais aucune poussée ni mobilisation de la structure.
[3] « Le recoil relance le dynamisme de l’architecture fasciale de façon spectaculaire en faisant lâcher les zones de plus forte rigidité ; en d’autres termes en déprogrammant par une impulsion mécanique et énergétique les dérèglements tensio-compressionnels qui s’y étaient installés.» Tarento M., Biotenségrité, Fascias, Ostéopathie, Sully 2021
Alchemy with three ingredients
It may seem surprising for an osteopath to limit his toolbox to only three techniques!
In fact, the three techniques described above are more than sufficient as they complete each other marvellously well.
- the tension test determines the tissue resistance to identify the osteopathic lesion.
- the balance test compares the tissue resistance to prioritize the osteopathic lesions.
- the recoil breaks the tissue resistance to correct the osteopathic lesion.
Using the same technique every day also has the advantage of continually training the hand. This daily repetition thus progressively develops the osteopath’s ability to solve all the problems encountered in common practice.
Therefore, with only three techniques, the LMO practitioner possesses an osteopathic method that is both unique and remarkably complete, a method that is efficient and applicable to all patients, regardless of their presenting complaint[1].
Of course, even though their association is ideal, there is no obligation to use these three techniques exclusively. You may very well integrate the tension test, the balance test and/or the recoil in your usual osteopathic practice, as a complement to the other means at your disposal. It is up to you to see and chose what works best for you!
[1] A « panacea » (from the Greek panákeia, with the root pan – everything and akos – remedy) in the original sense of the term: treatment technique that applies to all.
Eric Prat DO